 Posted by Behavioral Health Billing Solutions, LLC
Posted by Behavioral Health Billing Solutions, LLC
As always, Behavioral Health Billing Solutions, LLC (BHBS) is committed to bringing ongoing updates to Ohio Behavioral Health Providers.
style=”text-align: center;”>We also wanted to touch base and let all of our contacts know we are still here for you every day!
style=”text-align: center;”>We hope this post finds everyone safe and at home. If you are in the office or working in a potential exposure area, we thank you for what you are doing.
style=”text-align: center;”>Today I sent an email to an agency looking who is ready to make the change to a fully functional EMR. I sent the email below and thought it was important to share.
When I started BHBS in 2017, I wanted to be able to offer a software structure built with my knowledge (and our team), that could be used for a number of agencies to get on an EMR quickly and entirely proven from a billing perspective that could be very affordable and a much shorter implementation timeline. I looked at several, including Credible and oddly they wouldn’t share their plans for BH Redesign which was critical. We worked with Qualifacts to figure out a better way to deal with dual credentials and then decided to purchase a Qualifact’s “Carelogic” structure and partner with them. We built the structure from the ground up and then began accepting Associate agencies who are all set up on a HIPAA compliant level only accessible by them and BHBS. We currently have 23 Associate agencies on our structure. All are referrals for Behavioral Health Billing Solutions because we continually exceed their expectations. Because it is already built from a billing perspective, we are able to offer implementation at a fraction of the cost and the timeline is 4 – 6 weeks which is determined by your documentation needs. Our structure has available to new Associates all documentation already built for other Associates. These can be easily modified to meet your agencies needs or we can create it from scratch. That initial meeting determines your timeline for go live. We’ve had associates go live in 3 days (previous experience on CareLogic) – 6 weeks.
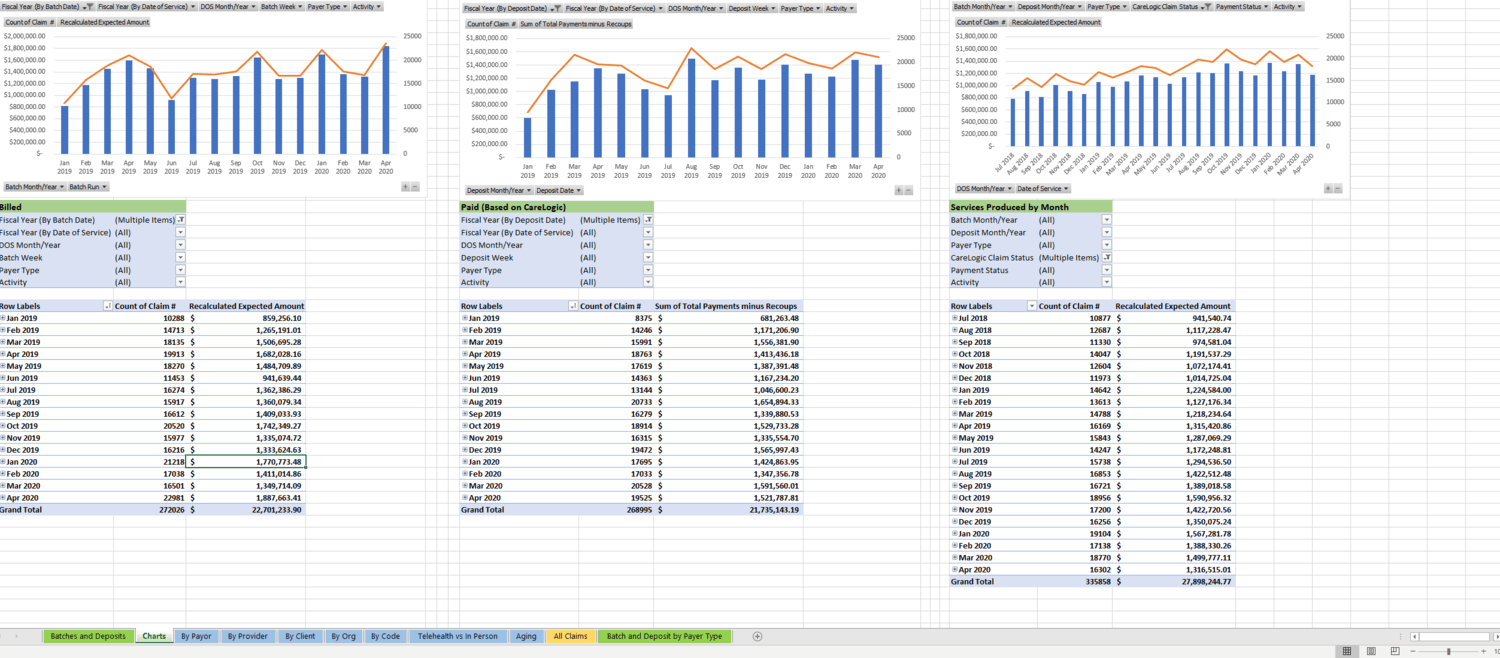
We are the system administrators for the structure and we offer billing services as well. The agencies we bill for have exceptional reimbursement rates and that will improve when ODM switches to a fiscal administrator in March 2021. Our billing services cover eligibility through financial reporting including incorrect denials/short pays to the MCO because after 2 1/2 years, there are still errors. I honestly have no idea how agencies not working with us are catching all of this because the process we have created is extremely complex and created by our team. Below is a sample of our financial report and some of the features it includes and tracks and is updated weekly for the clients we bill for.
style=”text-align: center;”>BHBS is proud to be a sponsor of the Ohio Council of Behavioral Health and Family Services Providers 2020 Virtual Training Series.

Ohio Council’s 2020 Virtual Training series continues. The next session is Tuesday, November 17th, 2020 from 10:00 am – 11:30 am and called “Understanding New Guidelines for Office & Outpatient E/M Services effective 2021”. Click here for the agenda.
To register for the event, click here.
Ohio Council Compliance Training Part Two presentation of the Virtual Training event hosted by The Ohio Council was held Thursday, October 29th, 2020 via webinar and included our own Behavioral Health Billing Solutions expert, Chelsea Kohler and I Am Boundless, Jennifer Riha.
Slides from the presentation are available here.
Feedback from the attendees has been extremely positive so we are looking forward to seeing additional trainings available over the next month.
Keep up to date with the latest Virtual Training dates and follow BHBS on Linkedin and Facebook for the latest updates.
In addition, Behavioral Health Billing Solutions, LLC is committed to keeping Ohio Behavioral Health agencies in the loop about the upcoming changes that will occur in the spring in conjunction with the MCO procurement process as well as other changes coming from ODM.
Last week, ODM announced updates to the BH manual and the primary change was the decision to allow interactive complexity to be billed for telehealth services effective November 15th, 2020.
The updated Medicare/TPL bypass now lists OTP services, now billable to Medicare and which codes are allowed to bypass. The revised list is available here.
In addition, changes were made to the allowed diagnosis list and is effective October 1st, 2020, an updated Diagnosis was released by the Ohio Department of Medicaid. Updated dated diagnosis’s are listed in RED here.
Another critical item that is now required effective October 1st, 2020 is OBHIS Outcome reporting. This is required for Mental Health and Substance Use Disorder providers. See below for more info.

On October 16th, HRSA hosted the HHS’ Provider Relief Fund and Behavioral Health Community webinar. This webinar introduces Phase 3 funding and demo’s of the PRF Application and Attestation portal.

A Step by Step guide is available here. In addition, Ohio Council provided a Shareholder Toolkit to share with your network. The Application and Attestation Portal is available here.
RFA: SOR 2.0 Application for Funding to Perform Evaluation, Training, Data Collection and Reporting
As a part of Ohio State’s Opioid Response (SOR) initiatives, the Ohio Department of Mental Health and Addiction Services (OhioMAS) seeks to partner with a college or university, medical organization or other organization with experience in grant evaluation and experience in achieving the required Government Performance and Results Act (GRPA) survey data collection and reporting for Ohio’s two SOR grants. The selected applicant will evaluate the grant performance, outcomes and impact to the State of Ohio and provide training and support to the SOR providers in collecting GPRA date; monitor and interpret data collected to determine whether an adaquate number of GPRA are completed and evaluate data integrity; identify and provide services and support to stakeholders that will promote the use of the GPRA; frequently interpret and report GPRA data, trends and highlights to OhioMAS, ADAMHS Boards and providers. Questions must be submitted to SORTreatment@mha.ohio.gov by 11:59 p.m. on November 6th. Responses to frequently asked questions will be posted on the OhioMAS Funding Opportunities web page. Applications must be submitted to SORTreatment@mha.ohio.gov by 11:59 p.m. on November 29th. Project implementation is expected to begin no later than December 4th.
View SOR 2.0 RFA (MHA-FY21-SOR-EvalDataRT-CommPL-10
And Ohio Council announced in yesterday’s update MHAS CARES Act Funding: Community Outreach and Education Initiative Funding Guidance and Application.
The Community Education and Outreach Initiative seeks to decrease stigma and connect Ohioans to support for emotional distress, mental health conditions or substance use challenges that are brought on or exacerbated by COVID19. The goal is for location partners to reach Ohioan’s to help them understand the signs and symptoms of emotional distress, mental health promotion strategies to manage emotional distress and pathways to get help when needed. A total of $2 million is available with individual awards capped at $25,000 per organization. Questions must be submitted to communityoutreach@mha.ohio.gov by 5:00 p.m. today, October 21st. Awards will be made of November 3rd for project completion by December 20, 2020. Click here to view the funding guidance and application.
We are also closely monitoring the upcoming changes in March 2021 in conjunction with MCO procurement. These updates include the following:
-
Implementation of a Fiscal Administrator. Although there is minimal information on these changes at this point, we do know that MITS will be upgraded to a modular system called the Ohio Medicaid Enterprise System (OMES). As part of this implementation, all BH claims and Prior Authorizations will be obtained and sent through this centralized location. See this link below for more detailed information.
-
Centralized Credentialing is also an important and exciting part of these upcoming changes. Once implemented, providers will only need to supply credentialing information ONCE to ODM, rather than go through a separate credentialing process with each Ohio Managed Care Plan. Please see this link for more details on this process.

