Behavioral Health Billing Solutions, LLC

Status update on the MCO carve in requested.
The challenges keep coming. This week was different from last only from the standpoint that I had time to review several client’s payments from the MCO’s. I found a multitude of incorrect denials or underpayments for services.
However, with that said, I have solid contacts with each MCO and they are immediately responsive and really want to correct issues and make this work.
Unfortunately, it may be too little, too late. We tried to say we (agencies) and they (MCO’s) weren’t ready and the results to date, in my opinion, have solidified that. Now agencies are starting to reflect the deficit in revenue due to credentialing, incorrect denials or payments, or an inability to bill as required.
A colleague, Sonda Kunzi, has sent out a survey requesting agencies experiences to date with this major change. Sonda has extensive experience in coding and behavioral health, as well as contacts to share these responses with. Take a minute and assist in impacting change before its too late.
Her request for information and the survey is posted below.
I’m sending out this email to gauge how things are going in the BH Redesign transition to MCOs processing of claims for my clients. I have heard from a few of you and I would love to get some collective feedback from those of you who have a minute to report on claims issues, delays of payments, credentialing issues, prior authorization challenges…or even if things are going great and everything is business as usual in terms of revenue flow.
If you have a minute or someone in your billing/finance department can take a minute to provide feedback please click on the link below to answer a simple 5 question survey. It should take less than a minute to complete. In addition, if you want to provide me any other feedback, just respond to this email with more specific information. I am also happy to share the overall results of the survey if you would be interested in receiving that information. Thanking you in advance for your participation.
https://lnkd.in/eEfX4pG
Best,
Sonda Kunzi CPC COC CPB CRC CPPM CPMA CPCO CPC-I Consultant/Owner Coding Advantage, LLC www.codingadvantage.com 216-978-2408 cell
Also an additional update from Sonda following our webinar on NCCI edits, QI compliance and Clinical appeals. Two important things to note about NCCI edits and how to utilize the modifers.
NCCI edit issue…
I believe I may have solved this mystery, with ODM assistance. I probably should have picked up on this early on!
For family therapy with psychotherapy Submit the 90846 or 90847 without a modifier and 90837 with the modifier
For group therapy with psychotherapy submit the 90853 without the modifier and the 90837 with the modifier
I believe if you submit as a corrected claim on any that have already rejected with the modifier on the wrong code, that should fix it.
NOTE: The trick is….if you put the modifier on the wrong code, you will not bypass the edit. Hopefully you can see the below screen shot. Whatever code is in the 2nd position (Column 2) in the NCCI table is the one that needs the modifier. Hope that makes sense.
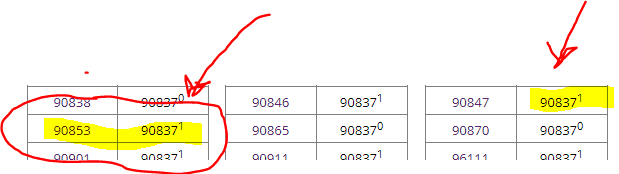
Also, we tested after the call and found that a Physician E&M with psychotherapy added does not cause psychotherapy provided by a different person to deny. However, as Sonda has told me several times, be sure to document WHY both are needed and to indicate medical necessity in the note.
In addition, I’ve had a number of requests from people who missed our webinar. I have posted all 3 presentations and a recording on the original list which can be found here.
In addition, Ohio Council has recently announced an interactive webinar, BH Managed Care Discussion of Billing/Coding concerns on Monday, September 17th from 1:00 pm – 2:30 pm. Targeted audience is CFO’s, billing staff and IT staff working through configuration issues. Let me stress that this series of webinars is available only to agencies that are members of Ohio Council.
This webinar series offers a platform to share updates from the state level and give providers an opportunity to identify claims and payment issues and identify system-wide issues that need to be elevated.
However, it is only offered to Ohio Council members. Considering that they are advocating for ALL agencies across Ohio, I recommend you consider applying for membership today. For membership requirements and benefits, click here.
Also, I would like to clarify who BHBS is and what our experience and services can do for your agency.
We are specialists in Ohio Behavioral Health Billing with high experience in Ohio BH Redesign and managing the MCO carve in.
Our range of services include all the critical aspects related to BH billing support, training and implementation support on a variety of software platforms.
Check out our website at https://bhbillingsolutions.com for more information.
In addition to our experience, we are a Trading Partner with Ohio Medicaid and an Affiliate Provider with Qualifacts for their Carelogic software system.
Being an Affiliate Provider with CareLogic allows us to offer a pre-built, fully
functional EHR that has proven to be successful in billing Ohio BH Redesign and MCO’s, and all other payers at a fraction of the cost and completed in a fraction of the time needed for a full, standalone implementation.
The CareLogic software system offers needed functionality that is just not available in other software programs. For more information on their software, check out their website.
In addition, we offer on-going training and support with experts in the behavioral health field. As a member of our structure, you get access to knowledge and information you simply can’t find with any other software or other affiliate provider in Ohio.
Our success within our current client base speaks for itself.
If your agency is currently in need of an EHR that works within Ohio or assistance with managing your current EHR, please contact us today.
Call 614-395-0136 or email teresaheim@bhbillingsolutions.com

